- [email protected]
- 0722 XXX XXX
2025
Annual Report
3 in every 5 preventable deaths are due to poor quality of care at health facilities in low-and middle-income countries in sub-Saharan Africa.
The key differentiator between the poor/low healthcare practice in SSA and the relatively higher/stronger healthcare practice in the US, Europe, or even India is the use of the science of quality improvement.
When frontline healthcare workers understand the science of quality improvement, they can study, analyse, and test solutions to the challenges in their processes and practices to make data driven decisions to improve care.
Kruk ME, Gage AD, Arsenault C, Jordan K, Leslie HH, Roder-DeWan S, et al. High-quality health systems in the sustainable development goals era: time for a revolution. Lancet Glob Health. 2018 Nov;6(11):e1196–252. https://doi.org/10.1016/S2214-109X(18)30386-3
Langley, G. J., et al. (2009). The Improvement Guide: A Practical Approach to Enhancing Organizational Performance. Jossey-Bass. (This is the foundational text for QI science).
Building a Movement for Quality Care
Strengthening Foundations Through QI-PS Theory
In 2025, the ACQUIRE Theory Leadership Course continued to build a strong foundation in Quality Improvement (QI) and Patient Safety (PS) for healthcare workers at all levels.
The course offered a comprehensive curriculum of 13 modules, covering core concepts in patient safety, leadership, teamwork, communication, improvement science, measurement, and population health.

reflecting a growing movement of professionals committed to improving the quality of care in Africa.

demonstrating increased engagement and the effectiveness of ACQUIRE’s structured learning model.
Strengthening Foundations Through QI-PS Experiential
In 2025, the ACQUIRE Theory Leadership Course continued to build a strong foundation in Quality Improvement (QI) and Patient Safety (PS) for healthcare workers at all levels.
The course offered a comprehensive curriculum of 13 modules, covering core concepts in patient safety, leadership, teamwork, communication, improvement science, measurement, and population health.

C-suite + QI teams involvement
C-suite leaders and QI teams worked side by side throughout the experiential program. Executives set direction, removed system barriers and protected time for teams to do improvement work, while QI teams carried out the day-to-day data collection, testing and documentation. This joint involvement ensured alignment between institutional priorities and frontline realities making projects move faster and increasing the likelihood of long-term adoption.
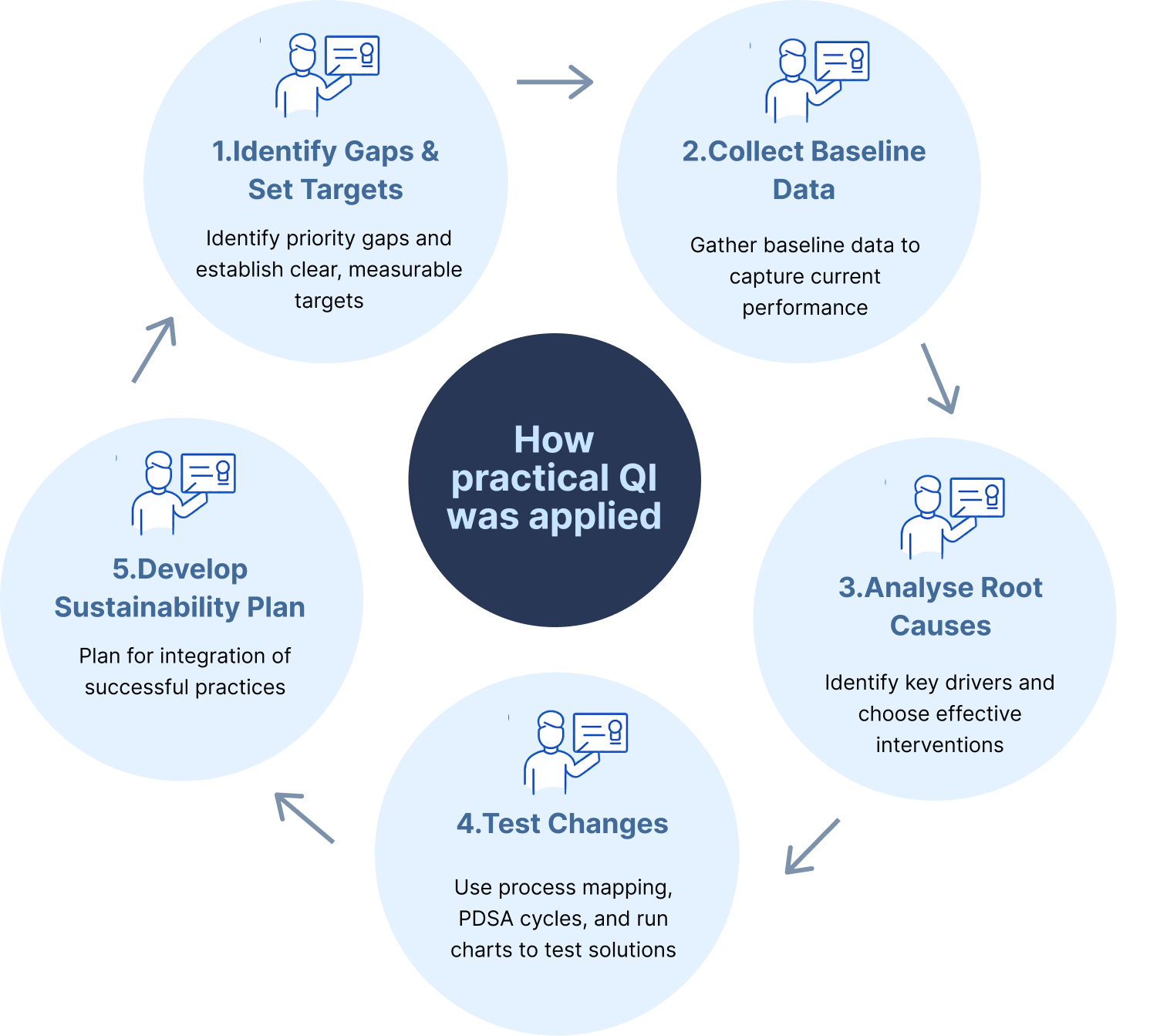
Facility-based improvement projects where teams used core QI tools—process mapping, root cause analysis, run charts, PDSA cycles and simple data audits—to diagnose problems, test small changes and measure continuous quality.
Target: Increase hand hygiene compliance among healthcare professionals from 65% to 80% within four months.

Root-cause analysis revealed barriers such as limited awareness, inconsistent commitment, poor monitoring, and inadequate availability of paper towels. In response, the team implemented a package of targeted interventions to strengthen accountability and drive behaviour change; including visual reminders, structured departmental conversations, timely dispenser maintenance, digital monitoring and feedback via Google Sheets, and recognition of hand hygiene champions. To sustain these gains, the team is integrating hand hygiene into management KPIs, embedding it in staff orientation and refresher trainings, and maintaining continuous monitoring through unit-based feedback and dashboards.
Target: Reduce patient waiting time in the cardiology outpatient clinic by 25%, cutting the average waiting time from four hours to three hours.

Root-cause analysis using process mapping and fishbone tools revealed underlying challenges including inefficient appointment systems, workflow gaps, and staff shortages. In response, the team introduced a series of targeted interventions to streamline patient flow and improve service efficiency; including a staggered appointment system to reduce congestion, patient engagement on appointment schedules, optimized staff allocation across clinics, and reminder messages to patients ahead of their visits. Within the first eight weeks, the team achieved a 15% reduction in waiting time and continues to work toward surpassing their 25% improvement goal. Their sustainability plan focuses on continuous patient education, routine data review, and active staff involvement to embed and maintain these gains.
Target: Reduce dental anxiety among male patients at Masango–Sanyane Dental Clinics by 30% from a baseline of 69.23% within eight weeks.

Root-cause analysis using surveys, Pareto charts, and fishbone diagrams revealed key contributors to patient anxiety, including an unwelcoming clinic environment, ineffective communication, and fear related to specific dental procedures. In response, the team implemented a set of high-impact interventions to enhance patient experience; including the introduction of chair-side conscious sedation, redesign of the waiting area to create a more welcoming atmosphere, staff training on identifying and supporting highly anxious patients, and providing clear explanations with scheduled breaks during longer procedures. Within six weeks, the team successfully achieved a 30% reduction in reported dental anxiety, and plans are now underway to scale these improvements to additional facilities across the region.
Target: Increase the percentage of pregnant women receiving comprehensive clinical checks and HB testing at their first ANC visit, moving from a baseline of 10% toward 100% coverage within three months.

Root-cause analysis highlighted significant gaps in ANC assessments, including limited provider skills, inconsistent use of clinical tools, and inadequate tracking systems; factors contributing to missed opportunities for early detection of anemia, a major driver of postpartum hemorrhage in Malawi. In response, the team implemented targeted interventions to strengthen service delivery; including weekly peer review and mentorship sessions for health workers, training for midwives and clinical officers on ANC assessment standards, distribution of standardized ANC checklists and tools, and the use of ANC registers to track and close gaps in missed assessments. By embedding these practices into daily workflows and aligning them with national SOPs, the Nasawa team is establishing a sustainable, system-wide approach to safer pregnancies and improved maternal outcomes.
Target: Reduce pressure injuries among at-risk patients in the medical–surgical and intensive care units by 60%, addressing a 2024 baseline where 22% of patients were affected.

Root-cause analysis using fishbone diagrams and Pareto charts revealed key contributors to pressure injuries, including gaps in staff training, inconsistent documentation, and limited availability of essential equipment. In response, the team implemented a series of targeted interventions to strengthen nursing care; including comprehensive staff training, routine and consistent skin assessments, provision of Braden Scale tools, and the introduction of ripple mattresses for high-risk patients. Within a few months, these efforts led to a significant decline in pressure injury incidence, from a median of 24.5 to 10. Their sustainability plan included incorporating the Braden scale to the admission and safety checklist as well as in an SOP, as well as putting a compliance system in place
The success of the 2025 ACQUIRE Experiential Leadership Course would not have been possible without the dedication, expertise, and unwavering support of our mentor-coaches. These individuals walked alongside the 22 QI teams throughout the 16-week journey; guiding problem analysis, strengthening QI skills, nurturing leadership, and ensuring that each team translated learning into meaningful, measurable improvement.
Their commitment to coaching, encouragement, and continuous follow-up played a pivotal role in building confidence within frontline teams and accelerating the adoption of evidence-based practices across participating institutions. We are deeply grateful for their professionalism, passion, and contribution to strengthening healthcare quality across the region.
Understanding the QI-PS Training Landscape
A Training Needs Assessment (TNA) revealed that although elements of Quality Improvement and Patient Safety (QI/PS) are present in both pre-service and in-service training, delivery remains fragmented and lacks standardization. Stakeholders expressed strong consensus on the importance of QI/PS training, emphasizing the need for practical, contextually relevant curricula, early integration into training programs, strong leadership support, and adaptability to diverse healthcare settings.

Generating and Sharing Evidence for Improvement
Fernandez JM, Kaderbhai H, Adams JL, Adam MB, Adam RD. Current management of skin conditions in Kenya: exploring teledermatology preferences and perspectives among providers. Int J Womens Dermatol. 2025 Feb 6;11(1):e196. doi: 10.1097/JW9.0000000000000196. PMID: 39917274; PMCID: PMC11801789.
Adam MB, Makobu NW, Mate K, Newman T, Donelson AJ. How Does QI Work? A Trust-Building Framework in African Healthcare: Primary Evidence from Kenya and Malawi. BMJ Open Quality 2025 May 28;14(2):e003330. doi: 10.1136/bmjoq-2025-003330. PMID: 40441735; PMCID: PMC12121567.https://bmjopenquality.bmj.com/content/14/2/e003330
Lelei F, Kynes M, Kynes A, Magayu M, Ndivo G, Sobekwa M, Adam M. Conference Reports Faith and Medicine Summit Held in Kijabe, Kenya. Christian Journal of Global Health 2025 Aug 29; 12(2): 78-83. https://cjgh.org/articles/10.15566/cjgh.v12i2.489
Kiaire PW, Okombo G, Makobu NW, Ambikile J, Adam MB. Patient Death and Nurses’ Coping Strategies: Perception of Nurses at a Tertiary Referral Hospital in Kenya. PLOS One (in press).
Okutoyi L, Godia PM, Jaoko W, Adam MB. Medical Error Reporting Among Healthcare Workers in a Kenyan Tertiary Level Hospital: A Knowledge, Attitude, and Practice Study. BMC Health Services Research (in press).
Dr. Mary’s Paper
Ruthpearls Presentation
Conversations That Shape Better Care

SESSION 1
Global Patient Safety Action Plan (GPSAP) 2021-2030: Translating Strategy into Action Across Africa and Beyond.
This session examines how African countries adapt the Global Patient Safety Action Plan to their contexts; strengthening leadership, systems, workforce, data use, and patient engagement.
SESSION 2A
Co-Producing Safer Care: Voices from the Ground, Patient and Provider Stories on Co-Creating Safety
This session highlights how patient and healthcare provider stories foster listening, challenge assumptions, build relational skills, and enable authentic co-production partnerships.
SESSION 2B
Co-Producing Safer Care: Voices from the Ground, Patient and Provider Stories on Co-Creating Safety
This session addresses barriers to co-production, offering practical frameworks, skills, and institutional support to embed it into everyday healthcare practice.
SESSION 3
From Silence to Safety – Translating Strategy into Action Across Africa and Beyond
This session explores current incident reporting mechanisms across African healthcare systems, identifies critical barriers and enablers to safe reporting, and maps approaches that can transform medical error reporting from punitive silence to transparency.
SESSION 4
Strengthening Capacity for Quality: Training Needs Analysis in Quality Improvement
Drawing from a Kenya multi-site study, the session showcases how training institutions, regulators, and ministries can work together to build a health workforce equipped to lead change.
SESSION 5
From Quality Assurance to Quality Improvement to Co-Production: A Journey Every Healthcare Worker Should Take
This session explores current incident reporting mechanisms across African healthcare systems, identifies critical barriers and enablers to safe reporting, and maps approaches that can transform medical error reporting from punitive silence to transparency.
SESSION 6
Exploring Generative AI’s Role in Enhancing Quality of Care: Exploring How Technology is Enabling Human-Centered Communication, Consent, and Care
This session is designed to spark a grounded, interdisciplinary dialogue on the responsible and impactful integration of Generative AI in healthcare communication, particularly in under-resourced settings.
SESSION 7
Celebrating Frontline Innovation: Scientific Poster Presentations on Quality Improvement
In this session, healthcare workers showcase quality and patient safety initiatives through scientific posters; promoting shared learning, recognition, and a culture of improvement across Africa.
Celebrating QI Champions Across Africa

Co-founder

Co-founder

Co-founder

Co-founder

Co-founder

Co-founder

Certified IRB Professional.

Certified IRB Professional.

Family Physician

Family Physician

M.D. MPH. M.B.B.Ch., FRCPCH, FCP (SA)

M.D. MPH. M.B.B.Ch., FRCPCH, FCP (SA)

Chairman of the Department of surgery, University of Nairobi

Chairman of the Department of surgery, University of Nairobi
| Institution | Country | Quality Improvement Project | |
|---|---|---|---|
| Orapa Mine Institute | Botswana | Needle Stick Injury Campaign: One Prick, Many Risks. | |
| Lobatse DHMT | Botswana | Proper Patient Records Management |
| Institution | Country | Quality Improvement Project | |
|---|---|---|---|
| Mbingo Baptist Hospital | Cameroon | Implementing Effective Documentation In Nursing Procedures | |
| Etoug-Ebe Baptist Hospital Yaounde | Cameroon | Assessing Patient Waiting Time And Strategies For Improving Service Efficiency In The Antenatal Clinic And Laboratory Of The Etoug Ebe Baptist Hospital Yaounde |
| Institution | Country | Quality Improvement Project | |
|---|---|---|---|
| Jimma University Medical Center | Ethiopia | Reducing Hospital Acquired Infections (Hai) By Increasing Hand Hygiene Compliance From 30% At Pediatric Hemato-Oncology And 10% At Nicu | |
| Cure Children’s Hospital | Ethiopia | Enhancing Equipment Longevity And Safety Through Rust Prevention In The Operating Room (Or) | |
| Landmark General Hospital | Ethiopia | Reducing Patient Wait Times In The Opd Through Process Improvement |
| Institution | Country | Quality Improvement Project | |
|---|---|---|---|
| Alimosho General Hospital | Ghana | Improving Hand Hygiene Compliance Among Health Workers | |
| FOCOS Orthopaedic Hospital | Ghana | Enhancing Emergency Preparedness: Improving Knowledge And Management Of The Crash Cart | |
| Techimantia Government Hospital | Ghana | To Increase Adherence To Appropriate Hand Hygiene Practices Among Nurses And Midwives From 45% To 85% Within Four (4) Months. | |
| FOCOS Hospital | Ghana | Hand Hygiene Compliance Improvement | |
| Asutifi North District Hospital | Ghana | Reducing Patient Waiting Times At The Asutifi North District Hospital | |
| Asunafo South District Health Directorate | Ghana | Improving Public Health Surveillance Reporting By Private Health Facilities | |
| Goaso Municipal | Ghana | Improving Breastfeeding Initiation By Caesarean Section Mothers Within 1hour At Goaso Municipal Hospital | |
| Regional Health Directorate, Ahafo | Ghana | Increasing The Number Of Maternity Unit Staff Skilled In Neonatal Resuscitation In A District Hospital ( From 0 To 20 Over 4 Months) |
| Institution | Country | Quality Improvement Project | |
|---|---|---|---|
| MOH | Kenya | To Reduce Hospital Acquired Pressure Sores Among Patients With Spinal Injury | |
| Coast General Teaching & Referral Hospital | Kenya | To Improve Magnesium Sulfate Medication Safety In The Management Of Severe Pre-Eclampsia And Eclampsia | |
| Vihiga County and Teaching Referral Hospital | Kenya | Hand Hygiene Promotion | |
| AIC Kijabe Hospital | Kenya | Optimizing Organizational Support Systems To Mitigate Burnout Among Employed Nurses | |
| Moi County Referral Hospital Voi | Kenya | To Improve Completeness Of Patient File Documentation In Adult General Wards From 20% To 75% By 20th April 2026 | |
| PCEA Hospital Kikuyu | Kenya | To Improve Hand Hygiene Compliance Among Healthcare Workers At Pcea Kikuyu Ahn Dialysis Unit From A Baseline Of 60% To 90%. | |
| Bristol Park Hospital, Nairobi | Kenya | Streamlining Outpatient Clinic Operations | |
| Alimosho District Hospital | Kenya | Reducing Delays And Enhancing Coordination In Inpatient Care | |
| Nazareth Hospital | Kenya | Enhancing Patient Satisfaction In Outpatient Services | |
| Kisumu CRH | Kenya | Improving Uptake Of Postpartum Family Planning (Ppfp) In Kisumu County | |
| Machakos County and Referral Hospital | Kenya | Implementing Sbar Communication Tool To Standardize Interdepartmental Communication By June 2026 | |
| Langata Sub-County | Kenya | Improving Staff Knowledge On Core Ipc Practices From January 2026 To April 2026 | |
| Kenyatta University Teaching Referral and Research Hospital | Kenya | Improving Patient Identification To Reduce Medication Errors | |
| Pandya Memorial Hospital | Kenya | Advancing Pandya Memorial Hospital From Safecare Level 3 To Level 5 | |
| Halisi Family Hospital | Kenya | Improving Waste Segregation Compliance | |
| Department of Health Services, Mombasa County | Kenya | Improving Tuberculosis Active Case Finding In Kaderbhuoy Dispensary By 80% | |
| Mwai Kibaki Referral Hospital | Kenya | Prevention And Reduction Of The Number Of Bedsores In Hospitalized Immobile Patients | |
| Mwai Kibaki Referral Hospital | Kenya | Enhancing Financial Sustainability For Inpatient Services At Mwai Kibaki Referral Hospital | |
| Moi Voi County Referral Hospital | Kenya | To Improve The Completeness Of Patient File Documentation In Adult General Wards In Moi Voi Hospital From 20% To 75% By 30th April 2026 | |
| Coptic Hospital | Kenya | Enhancing Accuracy And Completeness Of Iv Fluid Balance Chart Documentation | |
| AIC Kijabe Hospital | Kenya | Enhancing Clinical Training Quality Through Strengthening Preceptorship For Healthcare Trainee | |
| Pumwani Maternity Hospital – Nairobi | Kenya | Improvement Of Maternity Theatre Equipment | |
| Migosi Sub-County Hospital | Kenya | To Improve Community Pharmacy Model Uptake Among Plhiv In Migosi Subcounty Hospital | |
| MP Shah Hospital Nairobi | Kenya | Inpatient Discharge Turnaround Time At Kantaria Ward | |
| Migosi Sub County Hospital | Kenya | Improving Uptake Of Tb Preventive Therapy Among Healthcare Workers | |
| Mbagathi County Referral Hospital | Kenya | Strengthening Mental Health Screening And Referral Processes In Opd & Medical Wards At Mbagathi County Referral Hospital | |
| Mwai Kibaki Referral Hospital | Kenya | To Ensure That 90% Of All Routine Laboratory Test Are Released Within 90 Minutes Of Sample Receipt From Current 120 Minutes By End Of Second Quarter Ending 31st December 2025 | |
| PCEA Kikuyu Hospital | Kenya | Improving Patient Flow And Reducing Waiting Time In Consultant Clinics At Kikuyu Hospital | |
| Vihiga County Referral Hospital, Nairobi | Kenya | Improving Malnutrition Management In The Paediatric Ward | |
| Lamu County Referral | Kenya | Reducing Pre-Admission Waiting Times In A&E And Pediatric Departments To Enhance Patient Satisfaction And Care Continuity |
| Institution | Country | Quality Improvement Project | |
|---|---|---|---|
| Mercy James Centre for Paediatric Surgery & Intensive Care | Malawi | Reducing The Incidence Of Tissued (Infiltrated) Peripheral Intravenous Cannulas In Paediatric Intensive Care Unit (Picu) | |
| Reverend John Chilembwe Hospital | Malawi | Reducing Blood Sample Rejection Rates In The Hospital Laboratory | |
| St Gabriel Hospital | Malawi | Reducing Birth Asphyxia | |
| Bwaila Hospital | Malawi | Reducing Surgical Site Infections In The Operating Theatre | |
| Blantyre District Health Office | Malawi | Increasing Tb Preventive Therapy Initiation To Newly Diagnosed Hiv Patients |
| Institution | Country | Quality Improvement Project | |
|---|---|---|---|
| Alimosho General Hospital, Igando, Lagos | Nigeria | Reducing Patients Waiting Time In The General Out-Patient Department By 25%, From 1hour To 45minutes From The 15th Of January 2026 And 15th April, 2026. | |
| Massey Street Children’s Hospital, Lagos | Nigeria | Improving Staff Response To Emergencies | |
| Eti Osa Maternal and Child Centre, Lagos | Nigeria | Reducing Medical Laboratory Turnaround Time For Serum Bilirubin (Sb) And Full Blood Count (Fbc) | |
| General Hospital Lagos, Odan | Nigeria | Reducing Surgical Team Response Time To Surgical Patients In Emergency Units | |
| General Hospital Lagos Odan | Nigeria | Turnover Time Of Laboratory Investigations In Nephrology Clinic In Mopd |
| Institution | Country | Quality Improvement Project | |
|---|---|---|---|
| Benjamin Mkapa Hospital | Tanzania | Reducing Hospital Readmissions |
| Institution | Country | Quality Improvement Project | |
|---|---|---|---|
| St Francis Hospital Nsambya | Uganda | Enhancing Patient–Family Information Sharing And Documentation Practices | |
| Lubaga Hospital | Uganda | Increasing Reporting Of Incidents From 5 Incidents To 50 Incidents Per Month From January 2026 To June 2026 In Pharmacy Department Of Lubaga Hospital |
Scaling Impact in 2026 and Beyond
January – March
Experiential Leadership Course
120 hospitals implementing QI projects
Through Out The Year
April to Oct
Theory
5000 Learners on the e-learning platform
May to July
Curriculum
Testing QI Masters/short courses the e-learning platform
July to October
Experiential Leadership Course
120 hospitals implementing QI projects
August
QI Learning Forum
virtual